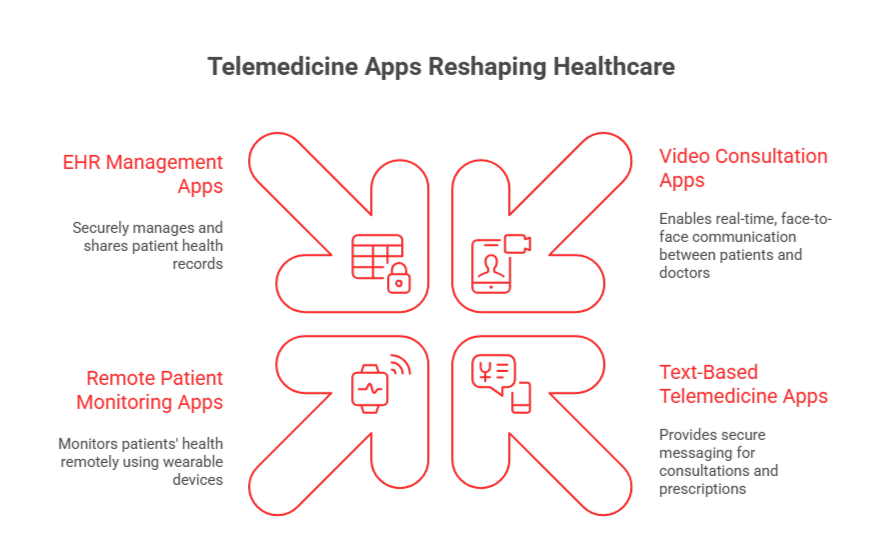
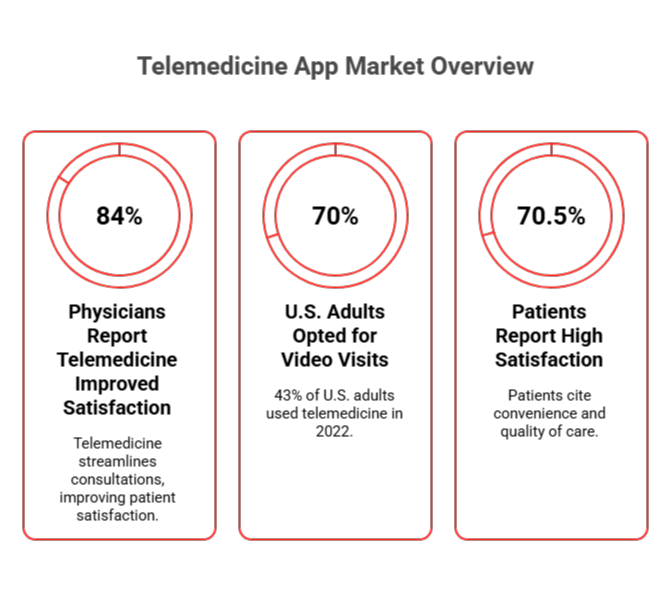
Telemedicine is transforming healthcare, and the demand for feature-rich telemedicine apps is skyrocketing. With the market set to grow from $124 billion in 2026 to $532 billion by 2034, understanding the must-have features is critical for anyone involved in healthcare app development or investing in telehealth solutions.
As telemedicine accounts for 25-30% of U.S. medical visits by 2026, your app must be scalable, secure, and user-friendly. In this post, we’ll break down the essential telemedicine app features and explore advanced tech like AI and machine learning to scale your platform.
Key Takeaways for Building a Feature-Rich Telemedicine App
Core Patient Features:
- Seamless Registration & Profiles: Quick, secure sign-up with multi-factor authentication for easy access to data.
- Video & Audio Consultations: HD, real-time calls across devices for instant provider access.
- Patient Portal & Records Access: Patients can view and manage their medical info directly.
Core Provider Features:
- AI-Powered Appointment Scheduling: AI optimizes appointment times and reduces no-shows.
- EHR/EMR Integration: Real-time access to patient records for better decision-making.
- Secure Messaging: HIPAA-compliant encrypted messaging for confidential communication.
Advanced Tech Integration:
- Remote Patient Monitoring & IoMT: Wearables monitor health continuously for proactive care.
- AI Chatbots & Symptom Checkers: 24/7 symptom assessment and triage for faster care.
Get Started with Your Telemedicine App Today
Ready to tap into the growing telemedicine market? Start developing your feature-rich app with the essential features that drive success and scalability.
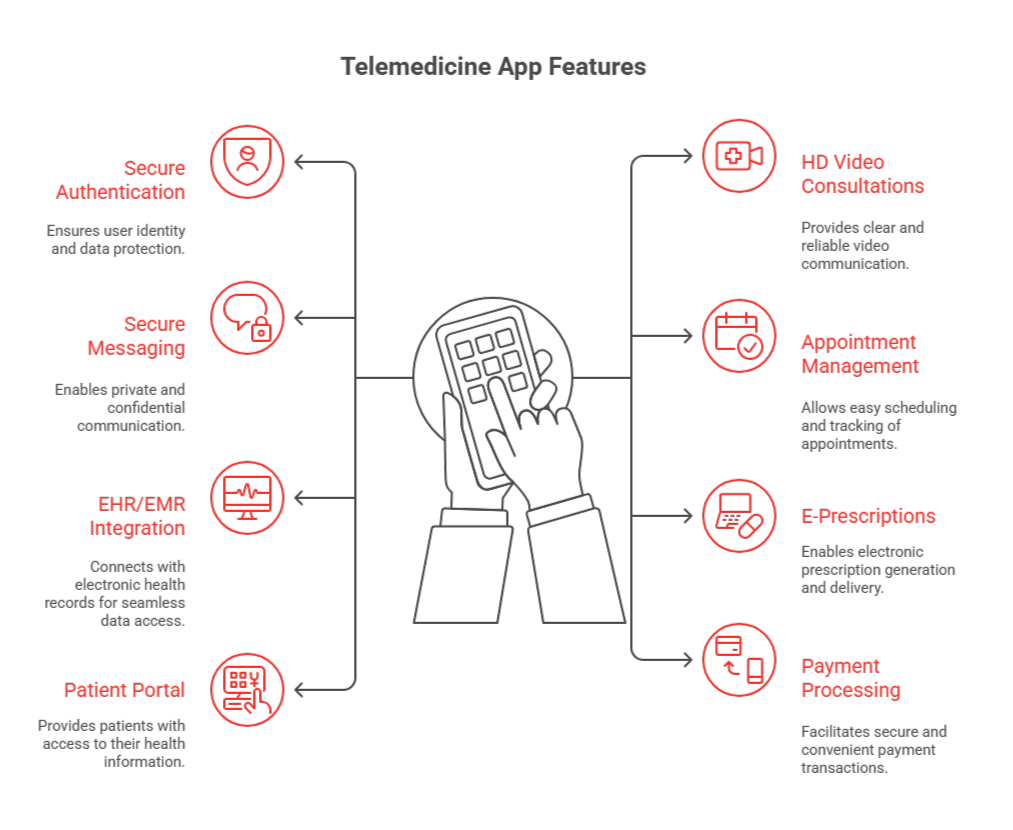
What Are the Core Features for a Telemedicine App?
When building a telemedicine app, certain features are non-negotiable. These essential elements form the backbone of a successful platform that meets both regulatory standards and user expectations. As healthcare software development trends evolve, the need for innovative solutions and new technologies becomes increasingly important in ensuring a seamless user experience and operational efficiency.
Here’s a breakdown of the must-have features and how they drive both user satisfaction and operational success:
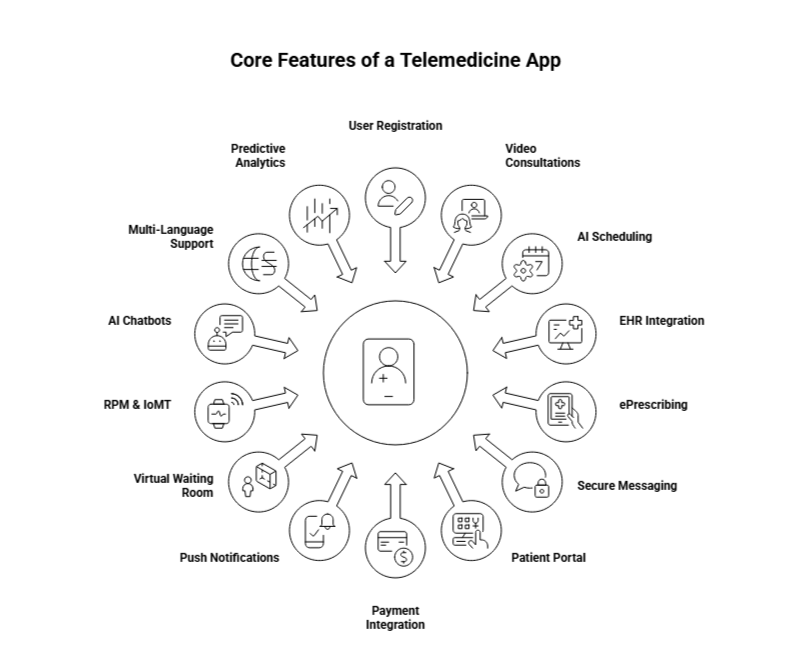
1. User Registration & Profile Management
- Secure Authentication: Multi-factor authentication ensures both patient and provider data is protected from unauthorized access.
- Profile Management: A comprehensive dashboard gives users immediate access to their health information and appointment history, streamlining the user experience.
For example, the Bradley County & Cleveland City Schools telemedicine program demonstrated how robust profile management and secure registration can dramatically improve healthcare access. By implementing school-based telemedicine across 27 schools, the districts saw a 1,365% increase in virtual visits, helping students receive care within minutes and eliminating transportation barriers.
2. Video & Audio Consultations
- Multi-Device Support: Seamless experience across desktops, tablets, and mobile devices ensures accessibility.
- EHR Integration: Syncs with Electronic Health Records (EHR) to enable easy scheduling and real-time consultation management, improving care coordination.
Telemedicine apps like Atrium Health’s Hospital-at-Home Program demonstrate how combining video consultations with in-person care and remote monitoring can improve patient outcomes and lower hospital costs, while still providing high-quality care outside traditional settings.
3. AI-Powered Appointment Scheduling
- Smart Scheduling: AI adjusts based on real-time calendar data, ensuring optimal appointment times for both patients and providers.
- Impact on No-Shows: AI scheduling helped reduce no-show rates by 54%, while Prospyr saw appointment completion rates increase from 11% to 36% for high-risk patients.
- New Patient Acquisition: Relatient’s 2024 results show a 47% higher new patient acquisition rate for organizations using intelligent scheduling, with 65% of self-scheduled appointments coming from new patients.
By reducing administrative tasks and improving scheduling flexibility, AI-powered systems can significantly enhance operational efficiency and patient experience, driving long-term value for telemedicine providers.
4. EHR/EMR Integration
- Seamless Data Exchange: Secure integration with EHR systems ensures real-time access to patient histories, lab results, and previous treatments.
- Impact on Patient Care: Studies show that integrating telehealth with EHR systems enhances patient outcomes and reduces overall medical costs.
By integrating EHR, telemedicine apps ensure providers can make informed decisions quickly, ultimately improving care continuity and patient satisfaction. Ochsner Health’s Connected MOM Program, for example, leverages EHR integration for remote monitoring of pregnant patients, improving maternal health outcomes and providing easier access to care for underserved populations.
5. Electronic Prescriptions (ePrescribing)
- Real-Time Checks: Integrates drug databases to automatically check for drug interactions or allergies.
- Automated Verification & Claims Processing: Automates the prescription and claims process, increasing efficiency and minimizing human error.
By simplifying prescription management, telemedicine platforms help reduce bottlenecks in patient care, leading to faster recovery times and fewer administrative errors.
6. Secure Messaging
- Encrypted Communication: End-to-end encryption ensures patient confidentiality and compliance with privacy regulations.
- Non-Urgent Follow-ups: Asynchronous messaging for follow-up questions helps doctors manage multiple cases more efficiently.
An encrypted messaging system allows for improved access to healthcare information without patients needing to visit the clinic, especially useful for non-urgent follow-ups and routine consultations.
7. Patient Portal & Medical Records Access
- Self-Service Access: Patients can view and manage their health information without needing to contact the provider directly.
- Document Sharing: Secure upload and sharing of medical documents between patients and healthcare providers.
By providing easy access to medical records, patients become more involved in their healthcare, improving outcomes and patient satisfaction. The Mayo Clinic’s virtual care system is a great example of this, offering patients 24/7 access to their health data.
8. Payment & Billing Integration
- Insurance Claims Processing: Automated insurance verification and claims submission save time and reduce human error.
- Transparent Pricing: Clear, upfront pricing models before consultations ensure patients understand costs, reducing surprises.
This feature also helps healthcare providers ensure they are compensated for their services efficiently, making the overall system more financially sustainable.
9. Push Notifications & Appointment Reminders
- Automated Reminders: Remind patients of upcoming appointments, lab results, or medication schedules.
- Personalized Alerts: Custom notifications based on patient preferences enhance engagement and care adherence.
The implementation of such reminders has shown to improve appointment attendance by over 30%, boosting both patient care and clinic revenues.
10. Virtual Waiting Room
- Triage Workflows: Automates the process of prioritizing patients, improving wait times and overall satisfaction.
- Reduced Wait Times: Enables real-time updates on wait times, giving patients a more controlled and less stressful experience.
Virtual waiting rooms have been shown to increase patient satisfaction by up to 23%, providing a seamless bridge between remote consultations and physical healthcare visits.
11. Remote Patient Monitoring (RPM) & IoMT Integration
- Real-Time Data: Wearable sensors and connected devices send continuous data, allowing healthcare providers to receive real-time insights and act swiftly if necessary.
- Chronic Disease Management: RPM is especially beneficial for managing chronic conditions like diabetes, hypertension, and heart disease. The ability to remotely track patient health leads to better management and fewer emergency interventions.
For instance, Atrium Health’s Hospital-at-Home Program integrates RPM kits to remotely monitor patients, improving patient outcomes and reducing the need for hospital admissions. Additionally, remote patient monitoring is a growing trend: 49% of healthcare professionals cite improved patient outcomes as the top benefit of RPM.
12. AI Chatbots & Symptom Checkers
- 24/7 Availability: AI chatbots offer round-the-clock symptom assessment, improving access and satisfaction. Accenture reports 80% of users prefer using AI for initial assessments.
- Symptom Triage: AI tools reduce wait times by 20%, helping patients quickly understand next steps in care.
- Accuracy & Efficiency: AI chatbots can diagnose with 76% accuracy, comparable to healthcare professionals in non-urgent cases.
- Increased Engagement: 63% of patients prefer AI chatbots for initial assessments, citing their convenience.
By integrating AI chatbots and symptom checkers, telemedicine platforms enhance patient engagement, reduce wait times, and streamline care delivery.
13. Multi-Language Support & Accessibility
- Health Equity: Offering multi-language services ensures that non-English-speaking patients receive culturally relevant and accessible healthcare. This is particularly crucial in diverse populations where language can be a significant barrier to care.
- Expanding Patient Base: Telemedicine apps with language support can cater to underserved populations, making healthcare more inclusive and equitable.
A study found that only 11% of patient portals are accessible in multiple languages, yet offering this feature could drastically improve patient engagement and outcomes. As the telemedicine industry grows, language support is becoming a key differentiator in reaching broader and more diverse patient populations.
14. Predictive Analytics & Population Health Management
- Proactive Care: Predictive analytics can identify early signs of chronic conditions or disease exacerbation, allowing healthcare teams to intervene before issues escalate.
- Optimizing Resources: With predictive models, healthcare providers can allocate resources more efficiently, focusing on high-risk patients and ensuring they receive timely care.
For example, HealthSnap utilizes predictive analytics to assist in chronic disease management, helping healthcare providers predict exacerbations and optimize patient.
Similarly, by anticipating health trends, predictive analytics can help healthcare providers manage population health more effectively, reducing hospitalizations and overall healthcare costs.
Integrating these essential features into your telemedicine app enhances both user experience and operational efficiency. While the telemedicine app development cost may rise with advanced tech like AI, the improved ROI makes it a worthwhile investment. For more insights on building a successful telemedicine platform, refer to our telemedicine app development guide.
How Can AI and Machine Learning Improve Telemedicine Apps?
AI and Machine Learning (ML) are revolutionizing the way telemedicine apps operate, enhancing diagnostic capabilities, optimizing workflows, and improving patient outcomes. Here’s how integrating AI and ML can elevate your telemedicine app:
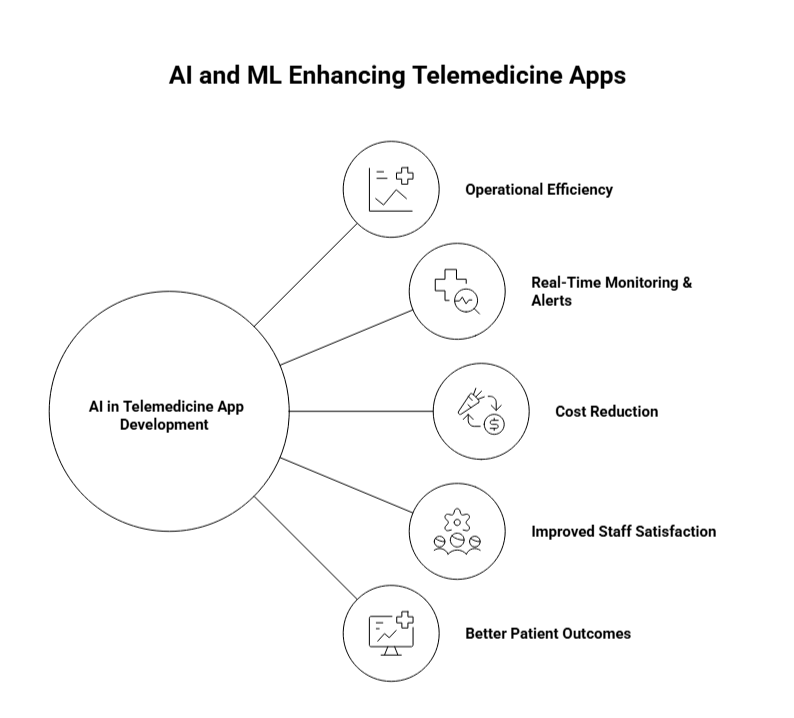
1. Enhanced Diagnostic Accuracy
AI’s ability to analyze large datasets and identify patterns far exceeds human capabilities, making it a game-changer in diagnostics. By integrating AI, telemedicine apps can improve the diagnostic accuracy of healthcare providers, helping them detect conditions that may otherwise go unnoticed.
- Precision in Diagnostics: AI-powered systems analyze medical images, lab results, and patient histories with exceptional accuracy, aiding in early detection of conditions like cancer, heart disease, and neurological disorders. In a recent study, AI algorithms were shown to be better than human doctors in detecting early-stage breast cancer, with a diagnostic accuracy rate of over 94%.
AI’s ability to enhance diagnostic accuracy not only improves patient outcomes but also reduces costly medical errors, making healthcare both more affordable and reliable. It is transforming telemedicine by offering more accurate diagnoses and quicker interventions, ultimately improving patient survival rates and the quality of care.
2. Clinical Decision Support
AI’s role in Clinical Decision Support (CDS) is crucial for real-time, data-driven decision-making. By utilizing AI-powered tools, healthcare providers can make informed decisions based on comprehensive patient data and evidence-based guidelines, all at their fingertips.
- Real-Time Decision-Making: AI analyzes patient histories, vital signs, and clinical data in real time, offering personalized treatment options and alerts when conditions change. For example, AI tools like IBM’s Watson for Oncology provide oncologists with evidence-based treatment suggestions by analyzing large volumes of medical literature and patient data.
By aiding in clinical decisions, AI helps healthcare providers stay up-to-date with the latest medical research, reducing diagnostic errors and improving treatment accuracy. For telemedicine apps, AI-driven decision support ensures that healthcare providers have the right information to deliver the best possible care, even from a distance.
3. Workflow Optimization
AI and Machine Learning aren’t just for patient care, they also optimize the administrative aspects of healthcare. These technologies automate mundane tasks, from appointment scheduling to medical billing, freeing up staff to focus on what truly matters: patient care.
- Automation of Administrative Tasks: Tasks like medical coding, patient scheduling, and claims processing can be automated using AI, leading to time savings and fewer human errors.
- Operational Efficiency: AI-driven systems can predict patient load, optimize provider schedules, and automate routine documentation, increasing operational efficiency across the board.
AI and ML integration have led to a 50% reduction in administrative costs in some hospitals. This not only boosts the bottom line but also improves staff satisfaction and reduces burnout.
By enhancing workflow automation, AI in telemedicine apps increases efficiency, reduces costs, and minimizes administrative errors, leading to a smoother, more streamlined healthcare delivery.
4. Real-Time Monitoring & Alerts
AI’s capability to provide real-time monitoring and alerts is a major benefit in telemedicine. Using AI-powered sensors, telemedicine apps can continuously track a patient’s health data and instantly alert healthcare providers if any critical signs are detected.
- Instant Alerts for Critical Findings: AI systems continuously monitor patient data, from vital signs to lab results, and trigger immediate alerts for anything abnormal, such as abnormal heart rhythms, elevated blood sugar, or signs of infection.
- Proactive Care: By providing real-time insights, AI allows healthcare providers to intervene before a condition worsens, leading to quicker response times and better patient outcomes.
In remote patient monitoring (RPM), AI-driven real-time monitoring has been linked to fewer hospitalizations, shorter hospital stays, and reduced mortality rates. AI in telemedicine apps ensures critical findings are flagged immediately, allowing healthcare teams to take swift action, which is key to improving patient survival and long-term health.
However, integrating AI and ML into telemedicine apps can impact the healthcare app development cost, particularly due to the advanced technologies and expertise required. While the initial investment in building AI-powered features may be higher, the long-term return on investment (ROI) can be substantial. AI and ML not only improve patient care and streamline operations, but they also reduce costs by preventing medical errors, improving diagnostic accuracy, and optimizing workflows.
Integrate AI for Better Patient Care
Enhance your telemedicine platform with AI-powered features like predictive analytics, real-time monitoring, and personalized decision support.
How Do Telemedicine Apps Ensure HIPAA Compliance?
HIPAA compliance is a critical aspect of telemedicine, as apps handle sensitive patient data that must be protected to maintain trust and meet legal requirements. With data breaches in healthcare costing an average of $6.45 million per incident, robust security measures are essential for protecting patient privacy. However, the healthcare app development cost often includes the need to incorporate advanced security features like encryption and role-based access control to meet HIPAA standards.
Here’s how top telemedicine apps ensure compliance:
- End-to-End Encryption
Telemedicine apps use AES-256 encryption to protect patient data during transmission and storage, ensuring it’s scrambled and unreadable if intercepted. A study shows 88% of healthcare organizations rely on encryption to meet HIPAA standards (HIPAA Journal), underscoring its importance in maintaining confidentiality. - Role-Based Access Control (RBAC)
RBAC ensures only authorized personnel can access patient health information, reducing the risk of unauthorized data exposure. Telemedicine apps with RBAC report 30% fewer breaches compared to those that don’t implement it. Real-time audit trails also track all interactions with sensitive data, enhancing accountability. - Continuous Monitoring & Audit Trails
To detect unauthorized access and identify security risks, telemedicine apps implement real-time monitoring and audit trails. These measures help mitigate potential vulnerabilities and safeguard data, as healthcare breaches are a major financial and reputational threat. Regular monitoring is crucial, as breaches cost healthcare organizations millions annually. - Staff Training & Incident Response Plans
Regular HIPAA training for staff ensures they understand the risks and protocols for handling protected health information (PHI). Well-trained staff can reduce the likelihood of breaches by up to 40%. In case of a breach, clear incident response plans help mitigate damage quickly. - Secure Data Storage & Backup
Telemedicine apps store patient data in encrypted databases, ensuring compliance with HIPAA’s data retention and disposal policies. This secure data storage and backup protect sensitive information from unauthorized access or loss. Telemedicine apps that adhere to these security guidelines face fewer legal challenges and retain patient trust.
In a digital-first healthcare world, HIPAA compliance is not just a legal obligation, it’s a key factor in protecting patient privacy and ensuring data security. By leveraging encryption, RBAC, audit trails, and real-time monitoring, telemedicine platforms can safeguard patient information and minimize the risk of breaches.
Ensure HIPAA Compliance with Expert Guidance
Protect patient data and maintain trust by ensuring HIPAA compliance. AppVerticals offers secure, compliant telemedicine solutions tailored to your needs.
Build Your Feature-Rich Telemedicine App with AppVerticals
Telemedicine is reshaping healthcare, and now is the perfect time to develop a powerful app that meets the demand for seamless, secure, and patient-centric services.
Whether you’re looking to integrate AI, enhance patient engagement, or ensure HIPAA compliance, AppVerticals has the expertise to turn your vision into reality. We offer custom-built telemedicine solutions with cutting-edge features that scale with your needs. Partner with us to build an app that’s both innovative and future-ready.
Build Your Scalable Telemedicine App with AppVerticals
Don’t miss out on the opportunity to create an innovative telemedicine platform. From EHR integration to secure video consultations, we can help you build a scalable solution.